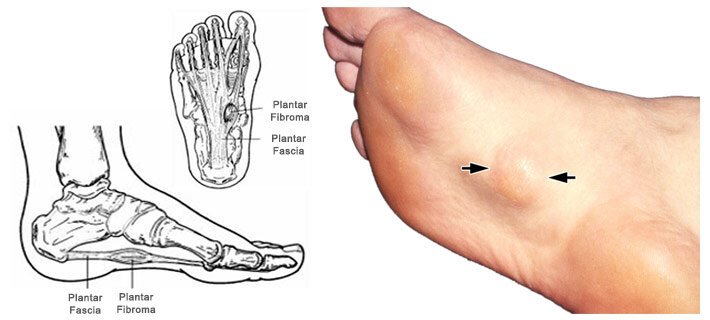
Image Credit: Vascular Health Clinics
“Your health is what you make of it. Everything you do and think either adds to the vitality, energy and spirit you possess or takes away from it. “ – Ann Wigmore
What Is Plantar Fibroma?
When a fibrous knot (nodule) develops in the arch of the foot, the condition is known as plantar fibroma. The nodule is embedded into the plantar fascia of the food, and is located in that band of tissue located in the base of the foot. The plantar fascia is embedded right in the arch of the foot. The degree of severity of plantar fibroma is variable, and can range from a benign condition, to one that is considered malignant and painful. Medical science is still currently investigating the root cause of plantar fibroma.
Signs & Symptoms
- A visible firm, lump in the arch of the feet
- In time the plantar fibroma has the tendency to grow over time
- Additional fibromas can develop in the region
- Occasional pain, depending on the severity of the fibroma. The location of the fibroma is right above the arch of the foot, and the patient can often experience pain when the patient wears shoes, walks barefoot or is standing up.
Diagnosis
The diagnosis of plantar fibroma is carried out by an orthopaedic surgeon. A foot and ankle orthopaedic surgeon will conduct a physical exam, in order to determine the current condition of the feet. During the physical exam, the surgeon will examine the base of the feet, and if there’s a fibroma, they will be able to classify the size. From the surface, the orthopaedic surgeon will note the physical symptoms of the patient. These include an indication of swelling, appearance of the skin, warmth or any redness in the base of the foot. Where necessary, there will be advanced imaging such as MRI’s that will be utilized in order to identify the inner conditions of the feet.
With orthopaedic conditions, in some instances, it is possible for more than one condition to exist that can cause a soft tissue mass in the foot. These conditions include foreign bodies in the foot, nerve tumors and even cysts. With the imaging technologies that currently exist, the orthopaedic surgeon will be able to rule out the additional condition, and identify if the root cause is attributed to plantar fibroma.
Treatment Options
Nonsurgical treatment may help relieve the pain of a plantar fibroma, although it will not make the mass disappear. The foot and ankle surgeon may select one or more of the following nonsurgical options:
- Steroid injections. Injecting corticosteroid medication into the mass may help shrink it and thereby relieve the pain that occurs when walking. This reduction may only be temporary and the fibroma could slowly return to its original size.
- Orthotic devices. If the fibroma is stable, meaning it is not changing in size, custom orthotic devices (shoe inserts) may relieve the pain by distributing the patient’s weight away from the fibroma.
- Physical therapy. The pain is sometimes treated through physical therapy methods that deliver anti-inflammatory medication into the fibroma without the need for injection.
If the mass increases in size or pain, the patient should be further evaluated. Surgical treatment to remove the fibroma is considered if the patient continues to experience pain following nonsurgical approaches. Surgical removal of a plantar fibroma may result in a flattening of the arch or development of hammertoes. Orthotic devices may be prescribed to provide support to the foot. Due to the high incidence of recurrence with this condition, continued follow-up with the foot and ankle surgeon is recommended [1]
ORTHOTICS:
After a series of consultations with your orthopaedic surgeon, you will be thoroughly examined and prescribed orthotics as part of your treatment regimen if the need arises. In acute situations your orthotics may be prescribed as your primary treatment, but where necessary they will be incorporated into a treatment plan to assist you with overall recovery.
What exactly do Orthotics treat?
Orthotics are recommended for conditions where feet aren’t ideally aligned. Individuals with flat feet for instance, are prescribed with orthotics to ensure that their feet alignment and arch development is enhanced. With the additional support added to the feet, the weight distribution of an individual is sustained via the critical cushioning that is provided to the feet. Where possible, orthotics are effective as preventative measures against eventual surgery.
What type of orthotics can I expect on the market?
There are different types of orthotics that your orthopaedic surgeon can prescribe for your condition. With a wide variety of materials available for your treatment, your orthotic will be custom made depending on your diagnosis.These treatments include:
- Arch Supports
- Insoles
- Heel liners
- Foot cushions
Medical innovation is an activity that is constantly being optimized. At the time of writing this article, carbon fiber, plastic and even silicone and cloth bases are utilized as materials for the orthotic. The aim is to ensure that the insole is flexible and cushioning. The design of your orthotic will be such that it may be either a full or partial insert.
What can I expect from my custom made orthotics?
As a general disclaimer, not all treatments are 100% effective but they do assist in improving the quality of life of the individual who they are prescribed to. There is no universal orthotic that will heal all foot conditions, nor will there be a guarantee that you’ll be immune to downstream surgery. The development of your foot treatment is dependent on the root cause of your condition. When it comes to your treatment, a multi fold consideration will have to be factored in. These focus areas will include:
- the training and experience of the person making the orthotic
- the doctor’s prescription
- the shoe in which a person wears them
- how often a person wears them
The key to success will be dependent on your situation. Stay positive however, and you’ll be able to identify the orthotic that is well fitted to your feet. With correct insertion, you’ll be able to alleviate your condition.
Physical therapy
Physical therapy is a medium that can be used to disintegrate the accumulated tissue in the foot. During your healing regime, your physical therapist will be able to develop a routine of strength training and stretching exercises that will improve blood circulation and stimulate cell growth. One of the enhancers of healing is blood flow to a site, and with the improved circulation, the inflammation caused by plantar fibroma can be relieved.
Surgery
With severe cases of plantar fibroma, surgical methods will be the best way to alleviate the plantar fibroma. As a treatment of last resort, the actions taken help to ensure that the patient’s comfort level is optimized. Once the surgery is completed, the recovery can take up to two months.
References:


