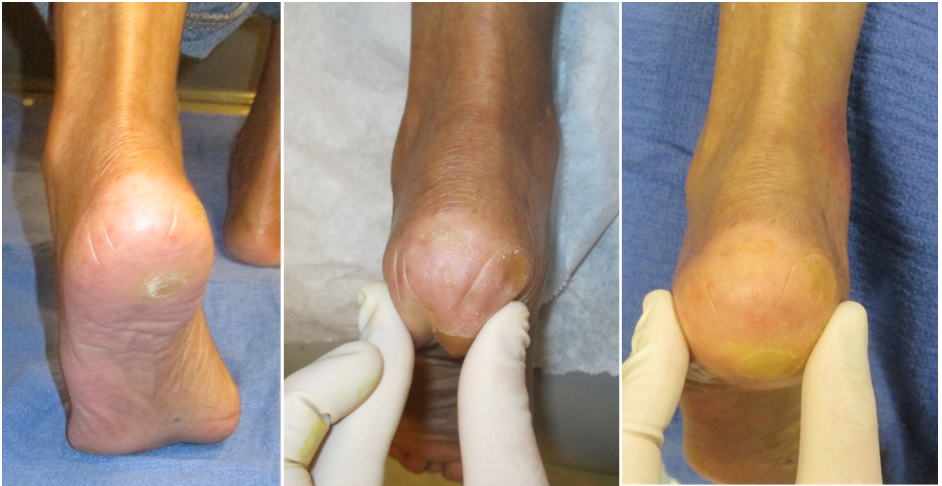
Image Credit: Podiatry Today
Authors: Gordon Slater| Tandose Sambo
“Our greatest happiness does not depend on the condition of life in which chance has placed us, but is always the result of a good conscience, good health, occupation, and freedom in all just pursuits.”- Thomas Jefferson
What Is The Pedal Fat Pad?
The mechanical design of the feet is actually quite complex, and each of the parts of the feet have their significant functions to perform. The pedal fat is the connective tissue that runs under the ball and heel of the feet. The pedal fat pad cushions the feet, and enables mobility to be a comfortable one for the individual. With the cushioning provided by the pedal fat, forces of friction, pressure and gravity are actually minimized during the activity of motion.
Pedal Fat Pad Atrophy therefore is the gradual degradation of the fat pad in the ball or heel of the foot. There are a variety of factors that are involved in the degradation of the fat pad, but for the most part aging is one of the influences of the onset of the condition. As a painful foot condition, the resultant thinning of the fat pad is what causes the patients to experience discomfort as the delicate connective tissue elements are exposed to higher external pressures. Internal inflammation and micro-injury is a result of the downstream effects of the pedal fat atrophy. Characteristics of pedal fat atrophy include [3]:
- Pan in the foot (Metatarsalgia) which becomes worse when wearing high heels or walking over a hard flat surface.
- Pain in the foot when a person is in standing position for extended periods of time. (62% of diagnosed sufferers report excessive foot pain after a long walk or long period of standing.)
- Feeling of the development of a mass or swelling in the foot/ heel.
- The ball of foot may become excessively thick due to callus formation.
Women have statistically been more prone to developing pedal fat atrophy than men. This observation, once studied in depth, identified that the lifestyles of women makes them more prone to specific foot conditions. Lifestyle choices such as the wearing of high heels or other tight footwear aggravates the feet, and increases the odds of callus formation and other degenerative foot changes.
Pedal Fat Pad Atrophy Influences:
Age: Age is directly correlated to the development of pedal fat pad atrophy. The ability to generate new cartilage and fat tissue, is one that is decreased with time. Studies have indicated that the changes are attributed to the limited blood flow to the area, as well as the reduction in stem cells to the area that can facilitate regeneration of new cartilage cells. As the cartilage and fat tissue regeneration is lessened, the bones will ultimately weaken. The degeneration of the pedal fat is a slow process that often begins in the mid-30’s and later surfaces in the patient’s medical history. As the decades progress, the pedal fat pad deteriorates until they are thin in later years such as the 60’s and 70’s.
Collapsed Bone: With the mechanical functions of the foot affected by the degeneration of the fat pad, there is a resultant effect on the long bones of the feet. With excessive vertical pressures on the feet, the bone damage odds can be increased.
Genetics: There are certain induced conditions that are contributors to the development of pedal fat pad atrophy. If a patient has a history of high pedal arches, the condition will also contribute to pedal fat degeneration.
Injury: Excessive physical activity that causes damage to the base of the feet, or other types of trauma that affect the feet, will contribute to the development of pedal fat atrophy. If trauma to the feet causes multiple fractures to the feet and requires surgery, in the aftermath of the condition, the patient will be prone to developing pedal fat atrophy.
Health Conditions: The presence of arthritis and diabetes are two health conditions that contribute to the development of pedal fat atrophy. Joint inflammation as a condition, will cause bone vulnerability in time that will cause impact on the feet. Diabetic have the potential to develop diabetic neuropathy. Patients with this condition do not have the ability to fully feel pain and pressure sensations. Downstream effects such as joint collapse will ultimately result in the development of pedal fat atrophy.
Treatment of Fat Pad Atrophy:
With all conditions, it is possible to have treatments that are either non-surgical or surgical in nature. For those with pedal foot atrophy, patients should make an effort to avoid excessive pressures on the feet. Since lifestyle conditions do contribute to the generation of pedal fat atrophy, it will be important to ensure that shoes are actually comfortable to wear. Minimize or eliminate the wearing of heels, if you have this condition. With exercises, take the time to engage in low impact activities that will optimize healing. With footwear, you can wear insoles that will provide cushioning for the feet. By minimizing the pressures on the feet, you will be able to protect the feet if your pedal fat atrophy is acute.
The utilization of Regenerative Medicinal efforts to create an environment that enables the restoration of healing of the body. The utilization of platelet rich plasma injections, which have shown great benefits in the treatment of osteoarthritis, is showing great promise in the treatment of pedal fat pad atrophy.
Conservative Treatment
With conservative methods involving treatments such as custom molded foot orthoses with padding, there are some conservative treatments that have proven to be effective in the treatment of pedal fat atrophy. They are countermeasures that are quite effective in the treatment of the patient. Essentially, they ease pain and prevent symptoms from worsening. With pressure relief available, the normal function of the foot can be restored.
The aim with the utilization of these foot orthoses, is to ensure that they have a cushion of 3-5 mm. A checklist of critical items to include in the treatment arsenal include:
*Viscoelastic Orthotic Devices
*Heel Cushions
*Heel Cups
*Inclusion of a cushioned top cover on shoes. Seek shoes with materials made of polyethylene foam.
Dermal injections are also currently being utilized in order to restore the internal cushion of the foot. Materials inclusive of poly-L-lactic acid and hyaluronic acid have been incorporated into the treatment of pedal fat pad atrophy. This methodology is still being investigated and is yet to be approved by the FDA.
.Autologous Fat Grafting
Autologous fat grafting is an emerging technology that is being used to treat pedal fat pad atrophy. This process involves a fat transfer from other parts of the body, and injecting those fat extractions into the bottom of the feet. The grafting process began approximately three decades ago, but with all technologies, there’s a curve that is involved in the understanding of the best approaches to utilize in patients in order to achieve results. With time, limitations of the technology were overcome.
Successful transfer of fats harvested from the abdomen of patients has proven to be successful in the restoration of patient pedal fat pads that were affected by previous injuries. With a thickening of the heel fat pad, the restoration of the plantar sole was achieved. The patients were able to resume normal weight bearing capability. This discovery among others has proven to be effective in the treatment of various pedal fat pad atrophy conditions.
CONTROLLED CLINICAL TRIALS
In a medical study[1], a randomized controlled trial was conducted to compare the fat grafting method with conservative methods. The study looked at the parameters of tissue thickness, pain and foot pressure changes with the inception of autologous fat grafting to the forefeet. The patients of the study were randomized, in order to receive either the fat grafts or conservative treatments. With baseline studies conducted at the start of the trial and in six month intervals till 18 months post treatment, the findings were noted.
The results for the study were actually quite impressive. With 11 of the patients in the study receiving bilateral injections, it was found that the patients with the injections demonstrated improvement in the functions of the feet according to the parameters that were established as the baseline for the trial. There was an improvement in the foot function, reduction of pain and the restoration of work/leisure activities. After one year, a notable improvement in all of these parameters was identified and quantified by the trial. The peak increase in tissue thickness was noted at six months post injections.
The controls group of the study showed the opposite effects of the study.The metatarsal tissue thickness showed a degradation across the first six months. The controls group at one year, had significantly greater foot pressures and forces than the patients with the grafts. The differentiation was showing that the treatment itself was effective.
While not fully effective in all patients, the procedure of fat grafting is a proven technology for the treatment of pedal fat pad atrophy. As a technique that improves the patients quality of life, the procedure is a minimally invasive procedure that treats fat pad atrophy.
References:
- Abstract: A Prospective Randomized Controlled Trial of Autologous Fat Grafting for Pedal Fat Pad Atrophy: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5147146/
- LERMagazine: https://lermagazine.com/article/management-of-painful-plantar-fat-pad-atrophy
- Morton’s Neuroma: https://bit.ly/3oLXUVh


