Image Credit: Regenexx
“To ensure good health: eat lightly, breathe deeply, live moderately, cultivate cheerfulness, and maintain an interest in life.” -William Londen
What is ankle fusion?
Ankle fusion is a surgical procedure that is utilized to fuse the bones of the ankle. Alternately known as ankle arthrodesis, the procedure is a procedure that is utilized in the treatment of ankle arthritis. Within the ankle joint is the intersection of bones such as the tibia, the talus and the calcaneus. Where a joint is formed, there is soft tissue such as ligaments and cartilage present, that provide mobility and cushioning to the joint. With time, cartilage of the joint is worn away. The increased friction results in pain, swelling and inflammation of the joint.
There are a variety of options that the patient can be advised by an Orthopaedic Surgeon, to be incorporated into the treatment and recovery plan. One such procedure is an ankle fusion surgery, that aims to stabilize the joint via the fusion of two or more bones in the ankle. The fusion surgery is designed to minimize the pain and swelling associated with the arthritic condition.
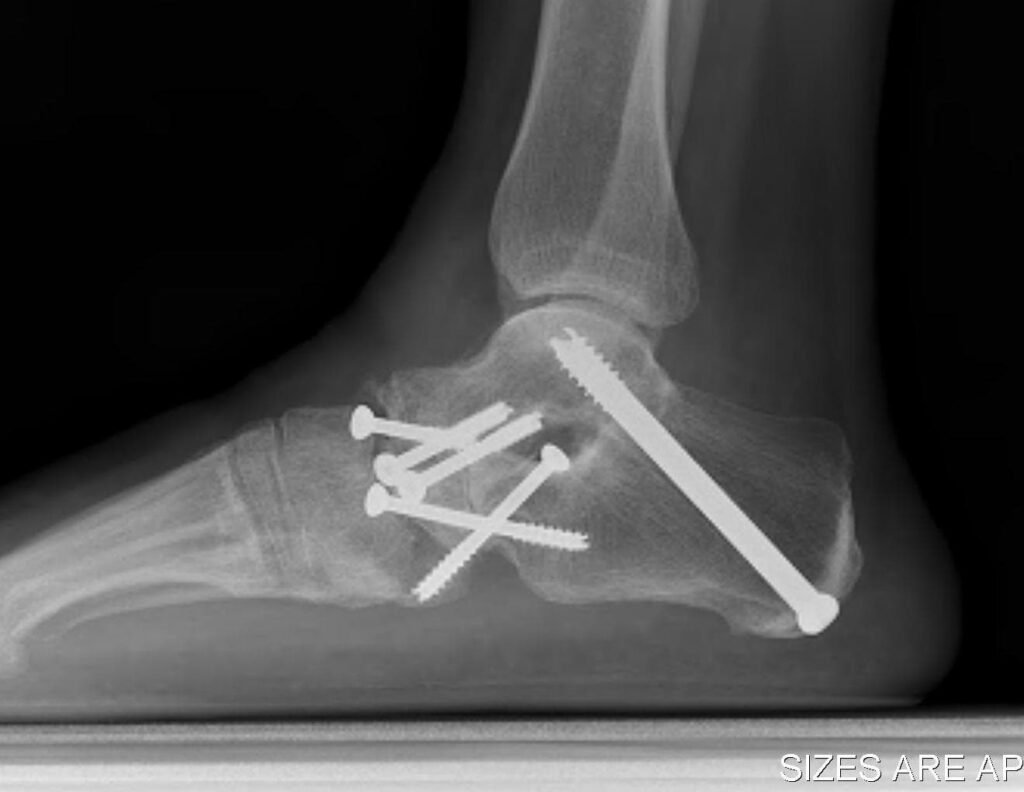
During the surgical procedure, a series of plates, nails and screws are utilized in order to unify the bones, and compress the joint. Where necessary, a bone graft will be utilized in order to complete the healing process. An ankle fusion, in some instances can be performed as a minimally invasive surgery.
There are a few conditions that can be treated via an ankle fusion. These include osteoarthritis, rheumatoid arthritis, or injury related conditions. For patients with mild to moderate arthritis, alternate treatments such as physical therapy will often be prescribed. Surgical methods are only for severe cases, as surgical procedures do have their associated risks. With ankle fusion surgery, there is often a reduction in the joint motion. The stability of the joint is often preferred by patients to the initial discomfort that is experienced from the arthritic condition.
Ankle Fusion Surgery
Your Orthopaedic surgeon will provide you with a detailed pre-surgical, surgical and post-surgical itinerary of activities that are geared towards ensuring the optimum treatment and recovery. In some instances, diet and medicinal changes will have to be made in order to ensure that you are in the best health for the surgical procedure. Patients who are smokers are often advised to stop smoking prior to surgical procedures, in order to ensure that their cardiovascular systems are at their peak.
Medical examinations will identify the nature of the ankle joint, and facilitate the hardware necessary to conduct the ideal surgical restorative process. During the surgical procedure, a team of specialists will be present to attend to your procedure. These specialists will include an aesthetician, your surgeon and the rest of the medical support staff. During the surgery, your surgeon will prepare the area, remove the joint cartilage and fuse the joint with the pre-designed hardware configuration. After the surgical procedure, your medical team will advise you on the best course of treatment. You will have a rest and recovery period for a few months, and a restorative phase that will be geared towards your mobility. Adequate pain treatment will also be prescribed.
ADVANCES IN TREATMENTS OF ANKLE CONDITIONS
There are some instances where the utilization of ankle fusion techniques, in the treatment of ankle arthritis may not be an optimal solution for a patient. Medical research is identifying these cases, and proposing the treatment enhancers that will enable the current limitations to be overcome. These treatments are often conducted at the small scale in animal tests, and then subsequently tested within a human model. Known as in vivo testing, it is possible to utilize the animal models to control the critical variables that will be scaled up into the human model. Orthopaedic in vivo tests are often conducted in small mammals such as mice or rabbits.
In this article, our focus area is on individuals who have bone defects. The presence of bone defects does pose an orthopaedic challenge that is currently being overcome in medical research. Patients with bone defects usually develop them, when a procedure such as ankle fusion isn’t initially successful. There are often revisional procedures implemented, and via their utilization the weaknesses in the bones are revealed. The leading method for restoring bone defects is autologous bone grafting. The procedure not only provides a structural restoration of the joint, there is also a biological restoration of the bone defect.
Autograft bones are alive, and they actually play a role in ensuring that relevant bone growth cells such as osteoblasts, osteocytes, and other critical minerals are present for the restoration of bone health. With the ability to induce the healing processes and facilitate the fusion of healing elements such as growth factors and matrix proteins, the appropriate parameters for bone growth are catalyzed and incorporated into the restorative process.
Complications with the autograft procedure includes pain, site defects from the point at which the graft was harvested, blood loss and surgical site infection. These complications are overcome by the utilization of bone morphogenetic proteins (BMPs). These BMPs are growth factor elements, and catalyze the differentiation of mesenchymal stem cells into the osteogenic cells that are necessary for bone growth. The protein recombinant human BMP-2 (rhBMP-2) is found to be especially useful, and induces the differentiation of mesenchymal stem cells into osteoblasts for bone growth, and chrondoblasts for cartilage restoration. Additionally, the protein is found to modulate vascular endothelial growth-factor activity. When utilized in the presence of a carrier like hydroxyapatite (HA), the optimum bone regeneration and healing conditions are enhanced.
Within the medical research conducted on both animal and human studies, use of rhBMP-2 to induce and improve bone regeneration for different types of bone defects in patients with ankle surgery is currently being investigated. Within animal studies on rabbits, studies did identify that the combination of rhBMP-2 with HA as a substitute for autogenous bone in a rabbit ankle-fusion model with a distal tibia bone defect, proved to be successful. With this knowledge, the treatment will in time be scaled up to a human model.
Medical science is an ever evolving field. As the knowledge of studies within the animal realm is understood, it is then possible to translate future medical innovations from the computational, theoretical realm into the actual real world applications. Eventually, knowledge like this will be utilized in order to treat arthritic conditions. Stay hopeful about your health.
Article References:
[1] Effect of Bone Morphogenetic Protein2/Hydroxyapatite on Ankle Fusion with Bone Defect in a Rabbit Model: A Pilot Study: https://www.researchsquare.com/article/rs-12767/v3
[2] Johns Hopkins Medicine: https://www.hopkinsmedicine.org/health/treatment-tests-and-therapies/ankle-fusion


