Image Credit: Podiatry Today
“Health is a large word. It embraces not the body only, but the mind and spirit as well; …and not today’s pain or pleasure alone, but the whole being and outlook of a man.”- James H. West
Medical Research In Space
Medical science is always an advancing field. While medical research on Earth is of benefit to the globe, there is an increasing amount of life-sciences based research that has, and is being conducted in space. The International Space Station is a hub for scientific endeavors including medical research, and aspects of study such as the investigation of factors that induce bone loss are influencing treatments on the planet Earth. What started off as an endeavor to apply research to maintaining the health of astronauts in space, is now being translated into the Earth equivalent, in order to help millions of patients who are suffering from conditions such as osteoarthritis.
There is a correlation between the impact of microgravity of space on astronauts’ bodies, and the muscular atrophy that bedridden patients exhibit with time. With minimal muscle use, the onset of muscle atrophy is induced, and understanding the mechanisms of a condition such as this in the microgravity environment, and combating it there, can also be translated to Earth related conditions. The scientific and biomedical gains of understanding how the body functions in space is proving to advance knowledge of bone physiology, bone physiology,cardiovascular and pulmonary systems, and neurovestibular studies. [3]
As more open-ended exploratory science is conducted, the more that we will know and apply to orthopaedic practice. With the ongoing research that NASA has conducted over the past few decades, a more general understanding of bone loss studied via the Gemini and Apollo missions and carried forward into the current missions, has led to current densitometric techniques that are utilized in clinics globally. Studies conducted during space flights indicated that up to 1-2% per month of bone loss is experienced in space, if there are no countermeasures to the root cause of this condition. With an understanding of the bone loss condition with weightlessness, there was also an identified difference of bone loss that occurred with time. The two types of bone loss identified were found to be cortical and trabecular losses.
With the knowledge gained, it is now possible to monitor the health of astronauts and with their constant medical tracking, patients are often rehabilitated in short order after they have returned to the planet. Terrestrial clinicians have also successfully been able to resuscitate patients who have experienced disuse of their bones and tissues due to a debilitating condition. Disused bone is actually absorbed into the body to some extent, and excreted via the urine. In treatment conditions, the restoration and remodelling of bone is often incorporated into the treatment plan. Space management of the body is conducted via exercise and dietary supplements. With ground based methods applying similar principles, bed rested patients have also recovered their bone density.
The translation of space related knowledge to the Earth is a great advancement, in a time when commercial crew activities are increasing on the International Space Station. Astronaut health studies have helped to advance the treatment of patients with amputated limbs, lower-leg fractures, ligament tears and conditions that result in minimal movement of the limbs. Early prevention during any of these conditions, has proven effective in preventing bone loss. Science is everywhere…from space to ground.
Joint Distraction Arthroplasty
Arthritis is statistically one of the most prevalent joint conditions. With the advent of medical innovation, the industrial trend is to facilitate the repair of joints, as an alternative to joint replacement in the advent of advanced cases of the health condition. Traditionally, it was found that regions of the body that were affected severely by arthritis were treated by joint replacement surgery. While studies showed that joint replacement was effective on regions of the body such as the knees and hips, the osteoarthritic ankle is a special breed.
The ankle is sensitive to therapies because of its location, and weight bearing capacity. In the case of ankle treatments, medical research has determined that the best therapies for joint restoration include the utilization of scaffolding technologies such as joint distraction arthroplasty. While lasting longer in terms of healing than joint replacement, the ultimate restoration of joint health is maintained in the long run.
Alternative Healing Therapies for Osteoarthritis
While acute treatments of arthritis involve therapies such as the use of mild pain relievers, insoles and ankle wraps, it is possible to utilize surgical treatments for the more advanced cases. Traditional methods of healing osteoarthritis include the process of fusion or arthrodesis. These methods facilitate internal scaffolding in order to improve joint integrity.
With an interconnected network of plates, and screws, the joint internal support is vastly improved and the ankle and leg are permanently affixed via this external support. The benefits of the procedure favor pain relief, but they are not aesthetically pleasing.
Joint Distraction Arthroplasty
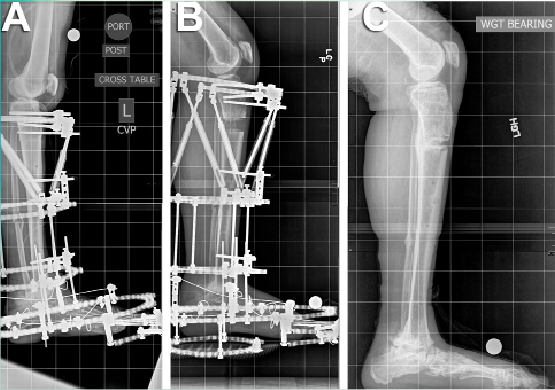
While both fusion and joint replacement have their pros and cons, it was identified that joint distraction surgery, via the procedure of joint distraction arthroplasty is an effective method of facilitating the body’s natural mechanisms in order to allow the joint to heal naturally. As indicated in the progressive X-rays highlighted in the image above, distraction arthroplasty involves:
How does the Distraction Arthroplasty Procedure Work?
Arthritis as a condition, involves the degradation of the articular cartilage that facilitates smooth joint operation. When your orthopaedic surgeon assesses your X-rays there will be cartilage loss that can easily be seen. As the joint stiffens, the patient will feel pain which affects their mobility. Since the joints are constantly in motion, healing is always slower than anticipated. By utilizing distraction arthroplasty, the body will be allowed to naturally heal itself. The procedure serves to release the joint contact, and the interbone spaces where the cartilage occupies is allowed to regenerate as there is renewed blood circulation to the area. What circulation does is facilitate healing.
How is the Joint Distraction Arthroplasty Surgery Conducted?
The distraction arthroplasty procedure is categorized as minimally invasive. A frame is erected around the joint to be treated. Via a configuration of rings, plates, hinges and screws as you’ll be able to see outlined in the image above, the ankle and leg are gently cradled. The application is executed surgically, and the removal is accomplished in a similar way. During surgery, if there are any additional joint adjustments to be made, they will be facilitated by your surgeon. If there are any bone spurs due to the joints rubbing together, they will be removed. Additionally, techniques to facilitate cartilage repair will be facilitated by your orthopaedic surgeon.
Healing Therapies
Medical Innovation is a process that is continuously evolving. During the healing process, mesenchymal stem cells from the patient’s bone marrow injected to the area. They jumpstart the healing process. Stem cells have the ability to adapt to their environment, and as a result they are able to morph into cartilage cells that will adhere to the bone surfaces and facilitate smooth joint restoration. In the past, scar cartilage was engineered by the surgeon via scraping the existing cartilage from the bones and allowing it to regenerate on its own. Scar cartilage is weaker than original cartilage, so it advantageous to utilize stem cells to help with the healing process. Embedded in a fibrin matrix, the cells are able to integrate with their environment and adapt to their new conditions.
Post Operative Care
The Distraction Arthroplasty process takes about two days. The first day is to facilitate the surgery, and the second day is to ensure that the patient can confidently manage to operate with the frame. A physical therapy session is usually prescribed, after which, the patient is discharged and allowed to return to their home life to heal. The frame is worn by the patient for ten weeks. They will be allowed to participate in regular hygiene activities such as showers, and also swim in pools. Careful treatment of the area where the skin is penetrated by the frame is also prescribed by the orthopaedic surgeon.
Research Credits:
- Joint Distraction Surgery: https://www.hss.edu/newsroom_joint-distraction-surgery-knee-ankle-osteoarthritis.asp
- Functional Analysis of Distraction Arthroplasty: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5270240/
- Nature: https://www.nature.com/articles/s41526-020-0095-y


